Periodontal Disease Treatment (Gum Disease)
Gum disease is a serious condition that affects people from all walks of life. Our dentistry provides periodontal services for all stages of gum disease to restore your oral health.
Periodontal Disease
Periodontal disease, periodontitis, and gum disease are all phrases used to describe an infection in the gums and bone surrounding your teeth. Healthy bone and gum structures help keep a tooth’s root intact. When food and plaque get trapped between the gums and teeth, it can lead to infection, resulting in gum disease. Periodontal disease is a very serious dental disease that affects many people. It is caused by bacteria from plaque formations on the teeth.
Gingivitis is an inflammation of the gums and one of the earliest stages of gum disease. Common symptoms of gingivitis include minor redness, swelling, or light bleeding of the gums. If left untreated, gingivitis turns into a more serious infection known as periodontal disease, which can lead to permanent structural damage.
Nearly half of all adults suffer from periodontitis to some extent—periodontitis is also referred to as gum disease and occurs when the gums are left exposed to harmful bacteria, tartar and plaque for an extended period of time. This can be caused by poor flossing habits and build-up between the teeth. If left untreated, it can progress and lead to bone and tooth loss.
-
What are the signs of periodontal disease or gum disease?
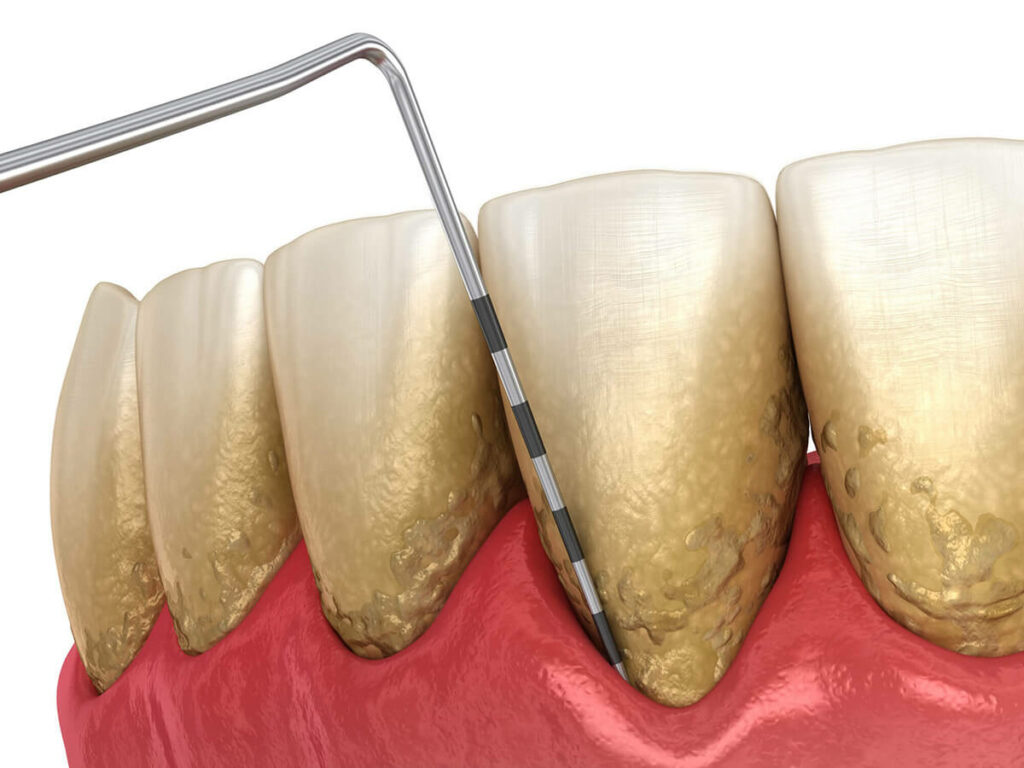
The earliest sign of periodontitis is an irritated gum line that might present some discomfort or bleeding when you brush, floss or have your teeth cleaned professionally. If not treated, the gums will start to retract and pull away from the teeth. This creates spaces between the teeth and gums called periodontal pockets that can quickly become filled with harmful accumulations. Your dentist will typically measure the depths of these pockets to determine how far the condition has spread and what treatment is needed to correct the problem. If gum disease eventually makes its way down to the jawbone and the connective tissues of teeth, the jawbone can deteriorate, and teeth can be lost.
Some of the most common symptoms of periodontal disease include:
- Gum recession
- “Long teeth”
- Tooth mobility (loose tooth/movement)
- Sore teeth when you chew/bite
- Spaces between teeth
- Deep pockets under your gums
- Visible bone loss on X-rays
- Heavy tartar buildup
- Bad breath
- Bleeding when you brush and floss
- Swollen, red gums
Please keep in mind that if you smoke, vape, or use tobacco products, you may not see the same symptoms as someone who doesn’t. Your tissues could look “healthy” due to the lack of bleeding or swelling, even if the disease is present.
-
How is periodontal disease or gum disease treated?
Periodontal disease, or gum disease, is effectively treated in two ways. Which treatment you receive depends on the severity of the gum disease.
Scaling and root planing are recognized as the standard treatment for periodontitis. The procedure is highly effective in managing the condition in its early to moderate stages. It also does an excellent job of reversing its harmful effects. When providing scaling and root planing treatment, your dentist will access the areas below the gum line and between the teeth and remove harmful accumulations of plaque, tartar and oral bacteria. Then the root surfaces will be smoothed out to prevent future accumulations. Your gums should then begin the healing process and eventually reattach themselves to the teeth.
The second treatment is called bone grafting and is often required when bacteria and plaque have reached the jawbone and caused some amount of deterioration and decay. Your dentist must surgically access the damaged jawbone in order to regenerate it. This is accomplished by applying proteins and artificial bone-like material to the areas of decay. This will help encourage new bone growth. Bone grafting is often a necessary step for strengthening the jawbone so that it can support dental implants to replace missing teeth.
-
How much does a deep cleaning cost?
We aim to provide high-quality dental care that’s affordable for our patients at each of our locations in Cincinnati, Batavia, and Lebanon, Ohio. Out of pocket cost for any procedure depends on your insurance coverage at the time of the procedure.
- Gum Infection Therapy (Perio Therapy): $272
Certain PPO plans may cover 100%
See All Office Fees -
What causes gum disease?
There are three usual causes of gum disease. The first and most common is chronic periodontitis. This occurs when oral hygiene is neglected and bacteria accumulate beneath the gum line, eventually turning into a hard substance called tartar. Tartar is not easily removed by brushing and flossing and requires professional cleaning. If left untreated the gums become inflamed and damaged and bone loss occurs. The second cause is aggressive periodontitis, this is believed to have a genetic component as it shows up in a small number of families. It moves quickly and can even be seen in children. The last and the rarest cause is necrotizing periodontal disease. This can occur in people with immune issues and or chronic diseases. The soft tissues and bone are compromised due to a lack of blood flow to the area.
-
What is gum recession?
Receding gums affect about half of Americans over the age of 50. But, young people can experience gum recession too. You may be genetically predisposed to gum recession. Some people are born with thin gums. Other times the environment might contribute to recession. Things like aggressive brushing, trauma, surgery, or ill-fitting partials can cause recession.
Treatment of Gum Recession
If you notice a tooth looks long or you experience sensitivity or pain when brushing and flossing, you could have gum recession. Be sure to come in and have one of the doctor’s take a look. If you have recession we can typically graft a small amount of skin from your palate and patch it over the receding area. The treatment helps protect the tooth from further damage. It is a minor procedure that can be done for a single tooth or multiple teeth depending on your need.
Your Comfort is Our Priority
We offer a variety of dental services to detect, diagnose, and treat dental issues while keeping your comfort a priority at all times. Learn more about our services or make an appointment with us today.



